Need to Know
- Do not eat or drink anything at least eight hours before the procedure
- If you take blood thinners, talk to your doctor beforehand about adjusting or stopping this medication
- Do not take aspirin or other pain relievers, such as Ibuprofen, for five days before the procedure
- If you have diabetes, ask your primary care doctor about adjusting your insulin dose
- Bring a list of all your medications and any allergies with you
Nice to Know
- This therapy is done in 2 or 3 stages. The first stage is a procedure to map your liver artery anatomy and to close artery branches that may go to bowel. A liver to lung shunt test is also performed to insure the lung will not be exposed to radiation.
- The actual delivery of the y90 beads is done several weeks later. Often there is one session to treat the right side of the liver and a separate procedure to treat the left side.
- These procedures tend to be very well tolerated with relatively mild side effects, the most prominent being fatigue for 4 or 5 days
- All of these procedures are done as a day patient at Hartford Hospital, with no overnight stay
Frequently Asked Questions
How Does Radioembolization Work?
The y90 beads produce beta radiation, which means it only penetrates about 2.5 mm (1/10th inch). That insures a high dose to the tumor and very little to the rest of liver or adjacent organs. The y90 becomes nonradioactive quickly, being half gone in 64 hours. You may go home and be around your family without posing a risk to them.
What Happens Before, During, And After Radioembolization?
You will be seen in our Farmington office for a consultation with an Interventional Oncologist before the procedure is scheduled to be certain this therapy is appropriate for you, and to be sure all your questions are answered. You will also have a consultation with a Radiation Oncologist at Hartford Hospital prior to the procedure.
The morning of the procedure you will be admitted to the hospital for administration of medications and IV fluids. Late morning or early afternoon you will come to interventional radiology where you will have the procedure. You will receive some IV sedation to make this a comfortable experience. After the procedure you will transported to Nuclear Medicine either for completion of the shunt study, or to document the treated part of liver, depending on which stage procedure you had.
You will be discharged later in the day.
How Should I Prepare For Radioembolization?
When possible, it’s good to have a family member or members accompany you to the consultation so that they also understand the therapy and can better support you during the process.
You will need to make arrangements with a family member or friend to bring you to and from the hospital for the procedure.
What Should I Bring To Radioembolization?
Everything will be provided for you at the hospital, but you may wish to bring reading material and or an MP3 player to pass the time.
What Are The Benefits And Risks Of Radioembolization?
The risks and benefits of the procedure vary greatly from patient to patient. They will be discussed with you in detail during your office visit consultation.

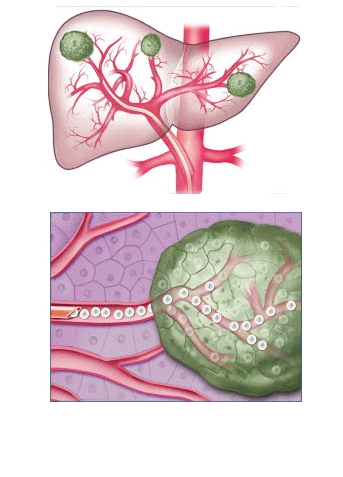 Cancer in the liver has been difficult to treat with external beam radiation therapy in the past because the normal liver is easily injured by radiation. Radioembolization is a technique that allows us to selectively subject cancerous tumors within the liver to high doses of radiation with little risk to the rest of the liver or surrounding organs. This is done, like with chemoembolization, through a tiny catheter or tube threaded into the hepatic artery (liver artery) from an anesthetized artery at the top of the leg. Tiny resin spheres, called Sir-Spheres, contain yttrium 90 (y90) are injected carefully through the catheter into the liver circulation. Cancer deposits have many more “parking spaces” for these radioactive spheres than do regions of normal liver tissue. Therefore, the cancer deposits receive far more radiation than does normal liver tissue. Cancers sensitive to radiation may be very effectively controlled with this therapy.
Cancer in the liver has been difficult to treat with external beam radiation therapy in the past because the normal liver is easily injured by radiation. Radioembolization is a technique that allows us to selectively subject cancerous tumors within the liver to high doses of radiation with little risk to the rest of the liver or surrounding organs. This is done, like with chemoembolization, through a tiny catheter or tube threaded into the hepatic artery (liver artery) from an anesthetized artery at the top of the leg. Tiny resin spheres, called Sir-Spheres, contain yttrium 90 (y90) are injected carefully through the catheter into the liver circulation. Cancer deposits have many more “parking spaces” for these radioactive spheres than do regions of normal liver tissue. Therefore, the cancer deposits receive far more radiation than does normal liver tissue. Cancers sensitive to radiation may be very effectively controlled with this therapy.






